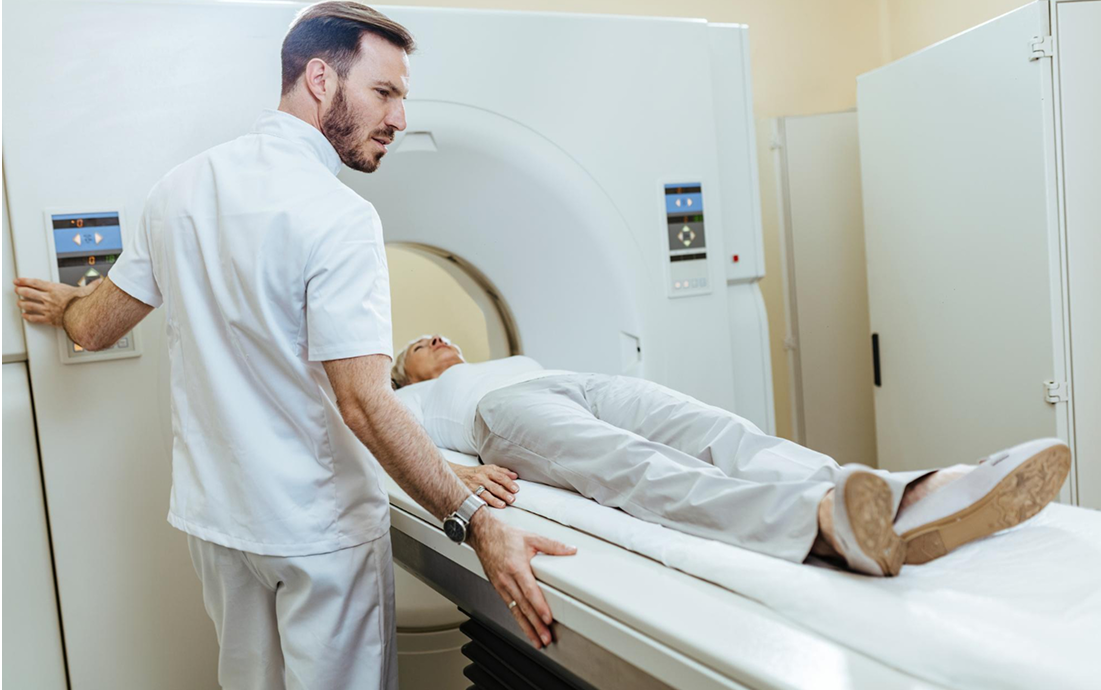
Welcome to Part 2 of the DocRBT Essentials series.
In this series, I’m breaking down the three outcomes that matter most to men undergoing robotic surgery for prostate cancer:
- Cancer control
- Urinary continence
- Erectile function
(In Part 1, we discussed erectile recovery. See the full article here: Preserving Erections After Robotic Prostatectomy: The DocRBT Approach)
Important: Radical vs. Simple Prostatectomy
Before we dive in, it’s important to clarify which operation we’re discussing, because recovery expectations are very different.
This guide is specifically for men undergoing a Robotic Radical Prostatectomy for prostate cancer.
Radical Prostatectomy
The entire prostate gland and seminal vesicles are removed to eliminate cancer. Because the prostate sits directly between the bladder and the urethra, this surgery requires a complete reconstruction of the urinary channel.
Simple Prostatectomy
A different procedure used for an enlarged prostate (BPH), where only the inner portion of the prostate is removed to improve urine flow.
Urinary control is a much bigger focus after a radical procedure, which is why surgical technique and recovery planning matter so much.
The Big Question: “Am I Going to Be Incontinent?”
For my patients in Arlington, the DFW Metroplex, and across North Texas, this is often the most pressing concern after a cancer diagnosis.
The short answer is that most men regain urinary control.
How quickly that happens depends on planning, surgical technique, and what you do after surgery.
Overviews
The Goal
Remove the entire cancerous prostate while preserving the structures that allow urinary control to return.
How We Do That
Protect the endopelvic fascia, preserve urethral length, perform a careful reconstruction — and allow the urinary channel to heal with as little irritation as possible.
What to Know Up Front
Early leakage is common. Long-term incontinence is not. Recovery happens in stages, and there are real, proven ways to improve the odds.
Where Urinary Control Really Comes From
Urinary continence is not controlled by a single muscle.
It depends on multiple structures working together, including:
- The bladder neck
- The external urinary sphincter
- The levator ani muscles
- The connective tissue that supports them (called fascia)
Fascia is the body’s natural scaffolding.
It’s a thin but strong layer of tissue that surrounds muscles, holds them in position, and allows them to contract together instead of pulling against one another.
In the pelvis, the endopelvic fascia helps anchor the pelvic floor muscles so they function as a coordinated unit. When this support system stays intact, urinary control tends to return faster and more reliably.
What Happens During Surgery That Influences Continence
Just like erectile preservation, continence preservation begins during the operation itself.
One of the most important — and often overlooked — factors is preserving the endopelvic fascia.
Why the Endopelvic Fascia Matters
The endopelvic fascia acts like a supportive hammock for the pelvic floor.
It allows the levator ani muscles to work together, tightening around and supporting the urethra when you cough, stand, or move. When those muscles contract as a unit, urinary control is stronger and more durable.
If this layer is overly disrupted during surgery, the muscles may still be present — but they don’t work together as efficiently. That can slow continence recovery.
Whenever the cancer anatomy allows, preserving this fascia helps maintain pelvic floor support and improves both early and long-term outcomes.
Other Surgical Details That Influence Recover
Bladder Neck Preservation – When it’s safe to do so, preserving the natural bladder neck supports earlier urinary control.
Preserving Urethral Length – The more healthy urethra that remains, the better the sphincter can function.
Gentle Tissue Handling – Limiting traction and avoiding unnecessary heat reduces temporary muscle and nerve dysfunction.
Careful Reconstruction – A tension-free, well-aligned reconnection of the bladder and urethra supports healing and continence.
No single step guarantees immediate dryness, but together these details make a meaningful difference.
What to Expect After Surgery: A Realistic Timeline
Some degree of leakage early on is normal, especially when standing, coughing, or during physical activity.
- Weeks 1–6: Gradual improvement as swelling decreases
- 3–6 months: Most men regain good urinary control
- Up to 12 months: Continued improvement in endurance and confidence
A smaller group takes longer, and a very small percentage may need additional treatment.
Why Pelvic Floor Exercises Only Work If Done Correctly
Pelvic floor exercises (Kegels) aren’t optional busywork — they’re rehabilitation.
In my practice, I give patients specific Kegel exercises to perform four times a day. When done correctly and consistently, they can significantly improve urinary control after surgery.
Kegels aren’t about squeezing as hard as possible. They’re about:
- Activating the correct muscles (imagine gently pulling the scrotum toward the belly button)
- Holding for the right amount of time
- Fully relaxing between contractions
- Repeating the pattern consistently
When done incorrectly or inconsistently, improvement is often slow at best.
The “Rule of 2s”: Simple Habits That Help Recovery
Once the urinary channel has begun to heal, bladder habits matter.
I recommend what I call the Rule of 2s:
- Try to urinate every two hours during the daytime
- Avoid drinking fluids within two hours of going to bed
This prevents the bladder from becoming overly full and reduces pressure on the healing urinary channel. Avoiding late fluids also improves sleep, which plays a real role in recovery.
Why I Use a Suprapubic Tube Instead of a Urethral Catheter
After robotic radical prostatectomy, the connection between the bladder and urethra needs time to heal.
Most surgeons use a urethral catheter (through the penis). I almost always use a suprapubic (SP) tube, which drains the bladder through a small opening in the lower abdomen.
This approach offers several advantages:
- Comfort: No one wants a plastic tube in their penis for a week
- Rest: The urethra can heal without constant irritation
- A “voiding trial”: We can safely test urination without re-inserting a catheter
Many patients find this approach far more tolerable during early recovery.
If Leakage Persists
If leakage continues beyond the typical recovery window, there are effective options, including pelvic floor therapy, medications, minimally invasive treatments, and surgical solutions when appropriate.
Persistent incontinence is treatable, and it’s addressed step by step.
The Bigger Picture
Robotic radical prostatectomy isn’t just about removing cancer.
It’s about preserving anatomy so the body can recover function. When the pelvic floor muscles and their supporting fascia are respected during surgery — and rehabilitation is done correctly — most men regain urinary control over time.
Take the Next Step in Arlington & DFW
If you’ve been diagnosed with prostate cancer, schedule a consultation so we can talk honestly about your recovery and create the right plan for you.
Call: 866-367-8768
Location: Urology Partners of North Texas | Arlington, TX
Book Online: Schedule Your Consultation
Watch: Continence Recovery After Prostate Surgery on the DocRBT YouTube Channel