
Elevated PSA Evaluation in Arlington & Dallas–Fort Worth
Hearing that your PSA is elevated can be stressful, leading to more questions than answers. We want you to know the truth: an elevated PSA does not automatically mean prostate cancer. It is, however, a critical signal that your prostate deserves expert attention.
As a dedicated prostate cancer specialist serving Arlington, Dallas, and Fort Worth, our goal is to make your evaluation clear, calm, and precise. We use advanced, evidence-based steps designed to avoid unnecessary biopsies while ensuring aggressive cancers are detected early—when treatment is most effective.
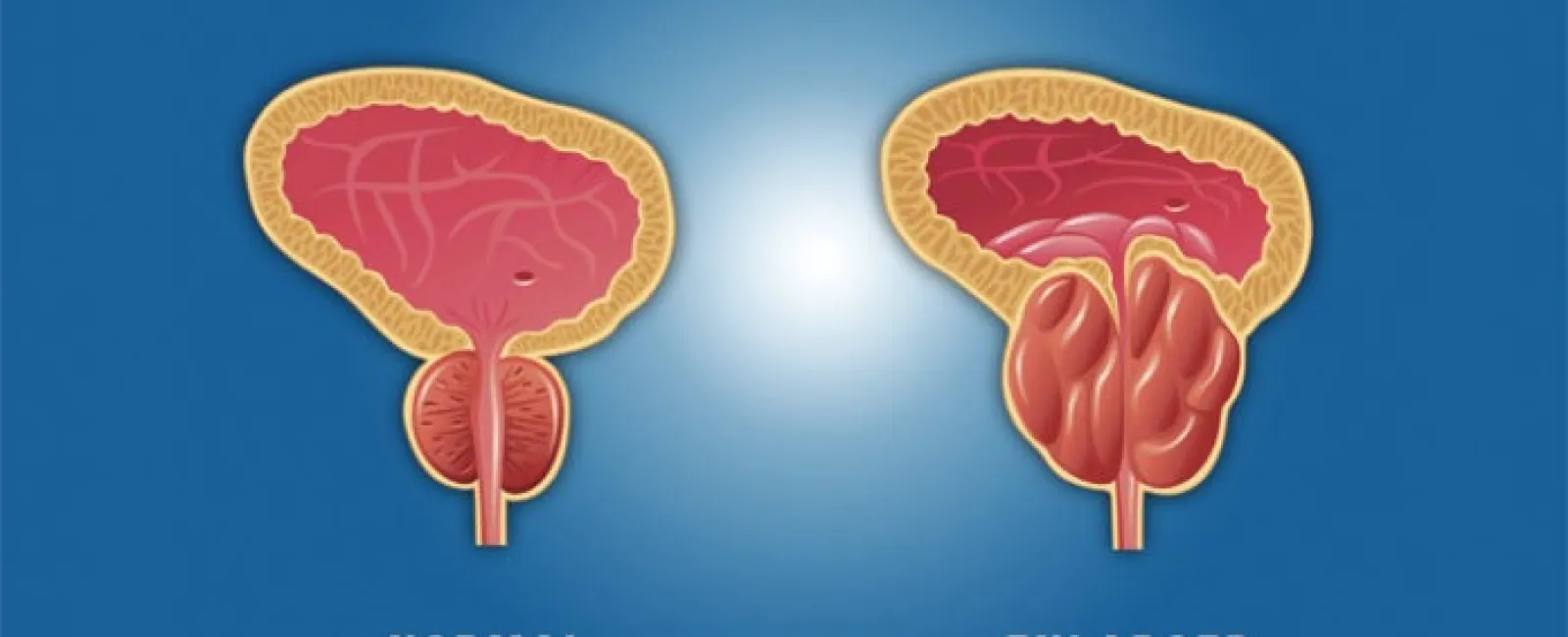
Illustration showing a normal prostate versus one enlarged due to elevated prostate-specific antigen (PSA)
What Is the PSA Test — and Why Does It Rise?
The Prostate-Specific Antigen (PSA) test measures a protein naturally produced by the prostate. Normally, only small amounts enter the bloodstream — but several conditions can raise PSA, not just cancer.
Common reasons PSA rises:
-
Benign Prostatic Hyperplasia (BPH)
An enlarged prostate that compresses the urethra. -
Prostatitis
Inflammation or infection that inflates PSA temporarily. -
Urinary tract infection or recent procedures
Even a catheter or recent ejaculation can cause spikes. -
Prostate Cancer
When cells become disorganized, more PSA escapes into the blood.
Think of PSA as your body’s “check-engine light.” It doesn’t always mean something serious is wrong — but it’s a sign you shouldn’t ignore.

Does an Elevated PSA Mean Cancer?
Most men with an elevated PSA do not have prostate cancer. Still, PSA remains one of our best early-warning tools.
The challenge is distinguishing a harmless rise from a true red flag. Instead of jumping straight to biopsy, I use a structured, evidence-based diagnostic pathway — combining PSA trends, MRI, PSA density, and molecular testing — to identify who truly needs further investigation.
Key PSA Red Flags We Look For
| Indicator | Concerning Threshold | Why It Matters |
|---|---|---|
| Absolute PSA | Persistently >2.5 ng/mL | May reflect prostate cancer, BPH, or inflammation. |
| PSA Velocity | Increase >0.7 ng/mL per year | A rapid rise can be more significant than the number itself. |
| PSA Density | PSA ÷ prostate volume | <0.15 = low risk. >0.15 = higher suspicion even with normal MRI. |
Why I use 2.5 instead of 4.0:
Many urologists still use 4.0 as the cutoff, but modern studies show that men between 2.5–4.0 can still harbor clinically significant cancers. That’s why I begin evaluation at 2.5 ng/mL — using today’s precision tools to decide the next step.
Your Step-by-Step Modern PSA Evaluation
Confirm the PSA and Perform an Exam
PSA can rise temporarily. I always repeat the test under standardized conditions (no infection, no ejaculation, no cycling).
A digital rectal exam (DRE) follows — quick, simple, and still one of the best ways to detect firmness or asymmetry suggesting cancer.
Get the Full Picture — Multiparametric MRI
The next step is mpMRI, which maps the prostate in exquisite detail without needles or radiation.
It uses three imaging sequences (T2, diffusion, and dynamic contrast) and grades each finding with PI-RADS 1–5:
- PI-RADS 1–2 = Low suspicion
- PI-RADS 3 = Equivocal (we refine using PSA density or urinary biomarkers)
- PI-RADS 4–5 = High suspicion → Biopsy recommended
MRI reveals what used to be invisible — helping many men safely avoid unnecessary biopsies.
Combine MRI with PSA Density and Molecular Testing
PSA Density = PSA ÷ prostate size (measured via MRI).
- PSA density < 0.15 + negative MRI → ~6% chance of significant cancer
- PSA density > 0.15 or positive MRI → Biopsy recommended
To further refine risk, I use ExoDx, SelectMDx, ConfirmMDx, and Decipher testing — molecular tests that analyze genetic signals for hidden cancers. This approach spares many men from unnecessary biopsies while identifying those that matter.
MRI Fusion Biopsy — Precision When Needed
If a biopsy is necessary, we make it count. MRI fusion biopsies overlay MRI images onto real-time ultrasound for precise targeting.
Using InVivo (transrectal) or Koelis (transperineal) systems, we combine targeted and systematic cores for maximum accuracy.
Reviewing the Pathology Report
I personally review your results face-to-face, explaining the Gleason Grade, tumor pattern, and whether the cancer is contained or aggressive.
If your biopsy is benign but PSA stays high, ConfirmMDx can detect hidden molecular changes in “normal” tissue to ensure nothing was missed.
Monitor or Treat — A Personalized Plan
If findings are benign, we continue PSA + MRI surveillance.
If cancer is confirmed, we create a treatment plan tailored to you — considering age, health, and tumor biology.
Options include Active Surveillance, NanoKnife Focal Therapy, Catheter-Free Robotic Prostatectomy, or Radiation with Barrigel Protection.
Modern vs. Old School PSA Evaluation
| Old Approach | Modern Approach (Dr. Bevan-Thomas) | |
|---|---|---|
| PSA Threshold | PSA > 4.0 = automatic biopsy | PSA > 2.5 → confirm + refine with MRI + molecular testing |
| Biopsy Type | Random 12-core biopsy | MRI fusion biopsy (targeted + systematic) |
| Treatment Model | One-size-fits-all | Personalized using PSA density + genomics |
| Results Timing | Weeks for results | Reviewed directly with Dr. Bevan-Thomas in ~5 days |
21st-century prostate care means less guessing, fewer needles, and more clarity.
Why Patients in North Texas Choose Dr. Bevan-Thomas
- 20+ years specializing in prostate cancer evaluation and treatment
- Among the earliest adopters of robotic surgery in the U.S. (since 2002)
- Comprehensive diagnostic tools: MRI, Fusion Biopsy, ExoDx, ConfirmMDx, Decipher
- Results personally reviewed and explained — not just posted to a portal
- One-stop diagnostic pathway in Arlington: MRI, biopsy, and follow-up under one roof

Personalized Prostate Cancer Treatment Options
At Urology Partners, there is no one-size-fits-all approach. Every plan is designed around your diagnosis, health, and lifestyle.
Active Surveillance
A proactive strategy for low-risk cancers—close monitoring with PSA, MRI, and periodic biopsy—to avoid unnecessary treatment while maintaining safety.
Focal Therapy with NanoKnife
Targets only the cancerous area, sparing healthy tissue and minimizing side effects.
Catheter-Free Robotic Prostatectomy
Minimally invasive surgical removal using the da Vinci system. Dr. Bevan-Thomas’ catheter-free technique improves comfort and recovery.
IMRT with Barrigel
Highly targeted radiation therapy with a protective hydrogel spacer (Barrigel) that shields nearby organs to reduce side effects.
Cryoablation (Cancer Freezing)
A precise, minimally invasive freezing technique that destroys cancer cells—even for patients who’ve had prior radiation.

Schedule Your Elevated PSA Evaluation
If you’ve been told your PSA is elevated, don’t panic — but don’t ignore it either.
The key is early, informed evaluation using precision tools that balance safety and accuracy.
- 866-367-8768
- 801 West I-20 Suite 1 • Arlington TX 76017
